Spinal Fusion Recovery: Physical Therapy vs. At-Home Exercises vs. AI Apps - What Actually Works?

After spinal fusion surgery, one question dominates every patient's mind: what do I actually do to recover properly?
Post-fusion rehabilitation is the structured process of rebuilding core stability, movement patterns, and spinal support after surgery - and the method you choose significantly affects how quickly and completely you recover.
Three main paths exist: formal physiotherapy, self-directed at-home exercise, and AI-powered recovery apps. Each has genuine strengths. Each has real limitations. Most patients do best with a combination - but knowing what each approach delivers (and where it falls short) is what lets you build a plan that actually works.
⚠️ Always follow your surgeon's and physiotherapist's specific guidance. This article provides general comparative information and is not a substitute for personalised medical advice.
TL;DR
- 🏥 Physiotherapy offers expert guidance, hands-on assessment, and safety - but is expensive, infrequent, and time-limited
- 🏠 At-home exercises are low cost and flexible - but lack progression logic, form feedback, and accountability
- 📱 AI posture apps offer personalisation and daily consistency - best used from month 3 onwards as a rehabilitation complement
- 🔄 Most successful recoveries combine all three at different stages
- ❌ Doing nothing - or relying on generic YouTube videos - is the riskiest approach of all
- 💡 The single biggest predictor of post-fusion outcome is rehabilitation consistency, not surgical technique
Why Recovery Method Matters More Than Most Patients Expect
Spinal fusion surgery permanently joins vertebrae to eliminate painful instability. But the surgery itself does not rebuild the muscles, movement patterns, or postural habits that protect the fused segment long-term.
That work happens in rehabilitation - and the quality of that rehabilitation directly determines whether you return to full function or continue living with pain.
Research in musculoskeletal rehab shows that patients who complete a structured, phased rehabilitation programme report significantly better outcomes at 12 and 24 months than those who had surgery without consistent follow-up exercise.
The fused segment is stable. Everything around it - the muscles, the adjacent vertebrae, the postural system - still needs deliberate rebuilding.
If you want to understand the full recovery timeline and what each phase involves, this guide to what spinal fusion is and what recovery looks like gives the complete picture before you compare methods.
Option 1 - Formal Physiotherapy
What It Is
Physiotherapy involves working with a qualified physiotherapist - either in a clinic or through home visits - who assesses your recovery, designs a progressive exercise programme, and adjusts it based on your response.
After spinal fusion, physiotherapy typically begins at 6-12 weeks post-surgery (Phase 2 of recovery), once your surgeon has confirmed sufficient early healing.
What It Does Well
- Clinical assessment: A physiotherapist can identify compensatory movement patterns, muscle imbalances, and pain sources that you cannot detect yourself
- Hands-on treatment: Manual therapy, soft tissue work, and guided movement correction are not replicable at home
- Safety: A qualified clinician monitors for warning signs - nerve symptoms, unusual pain patterns, or movement errors that could stress the fusion site
- Structured progression: Programmes are designed with clear phase logic, not random exercises
- Psychological support: Regular clinical contact reduces fear-avoidance - the common post-surgical tendency to avoid movement out of fear of re-injury
Where It Falls Short
- Cost: Private physiotherapy sessions typically cost £50-£120 per session in the UK, or $80-$200 in the US. A full post-fusion programme may require 20-40 sessions
- Frequency: Most patients see a physiotherapist once or twice per week. The other 5-6 days are largely unsupported
- Availability: NHS physiotherapy waiting lists can stretch to months. Insurance coverage varies significantly
- Compliance gap: Exercises assigned for home practice are frequently done incorrectly or not at all without supervision
💡 Key Insight: Physiotherapy is most valuable in the early structured phases (weeks 6-16) when clinical assessment and hands-on correction are genuinely necessary. It becomes less efficient - and less affordable - as the primary tool for the long maintenance phase of recovery.

Option 2 - At-Home Exercises
What It Is
Self-directed home exercise involves following a programme - from a physiotherapist's discharge sheet, an online resource, or a written guide - independently, without real-time supervision.
For post-fusion patients, this is often the default mode of recovery after the formal physiotherapy phase ends.
What It Does Well
- Accessibility: No appointments, no travel, no cost per session
- Flexibility: Exercises can fit around work, family, and energy levels
- Daily frequency: Unlike clinic visits, home exercise can happen every day - which is what the recovery actually requires
- Low barrier to entry: Basic equipment (a yoga mat, a resistance band) is sufficient for most post-fusion exercises
Where It Falls Short
- No form feedback: Incorrect exercise technique during post-fusion recovery is not just ineffective - it can load the spine incorrectly and create new problems
- No progression logic: Generic programmes do not adapt as your strength and mobility improve. Most people plateau or regress without realising it
- No accountability mechanism: Motivation naturally declines during months 3-6, when the acute phase is over but full recovery is far from complete
- Wrong exercises: Generic back pain programs found online are frequently inappropriate for post-fusion patients. Exercises that are safe for non-surgical back pain may be dangerous after fusion
For at-home exercises to work safely after fusion, the programme needs to be specifically designed for post-surgical recovery - not repurposed from generic back pain content. This phased breakdown of exercises after back fusion outlines what safe, appropriate at-home work actually looks like at each stage.

Option 3 - AI Posture and Recovery Apps
What It Is
AI-powered recovery apps use your smartphone camera to analyse posture, identify movement compensations, and deliver personalised exercise programmes based on your specific profile - not a generic template.
Backed AI is designed around exactly this model: camera-based posture analysis, personalised corrective exercise delivery, and daily habit-building reminders that keep patients consistent during the long middle phase of recovery.
What It Does Well
- Personalisation at scale: Unlike a generic home programme, an AI app adapts to your posture patterns, progress, and current limitations
- Daily consistency: Short, guided sessions replace the willpower requirement of self-directed exercise - the single biggest failure point in at-home recovery
- Postural compensation detection: Post-fusion patients frequently develop compensatory patterns - leaning, rotating, shifting weight to avoid discomfort. AI posture scanning identifies these before they become structural problems
- Progress tracking: Objective data on posture improvement and exercise completion replaces the guesswork of self-assessment
- Cost efficiency: A monthly app subscription costs a fraction of a single physiotherapy session - and delivers daily, not weekly, support
Where It Falls Short
- Not appropriate in early recovery: AI apps are not a substitute for clinical physiotherapy in the acute phase (weeks 1-12). They are not equipped to replace hands-on assessment, manual therapy, or surgical monitoring
- No emergency intervention: If something goes wrong, an app cannot assess or respond in real time the way a clinician can
- Requires baseline capability: Most AI recovery tools work best when the user has already completed the foundational physiotherapy phase and can move safely and independently
The optimal entry point for AI-assisted recovery after spinal fusion is typically month 3 onwards - when the initial clinical phase is complete and the challenge shifts from safety to consistency.
Head-to-Head Comparison
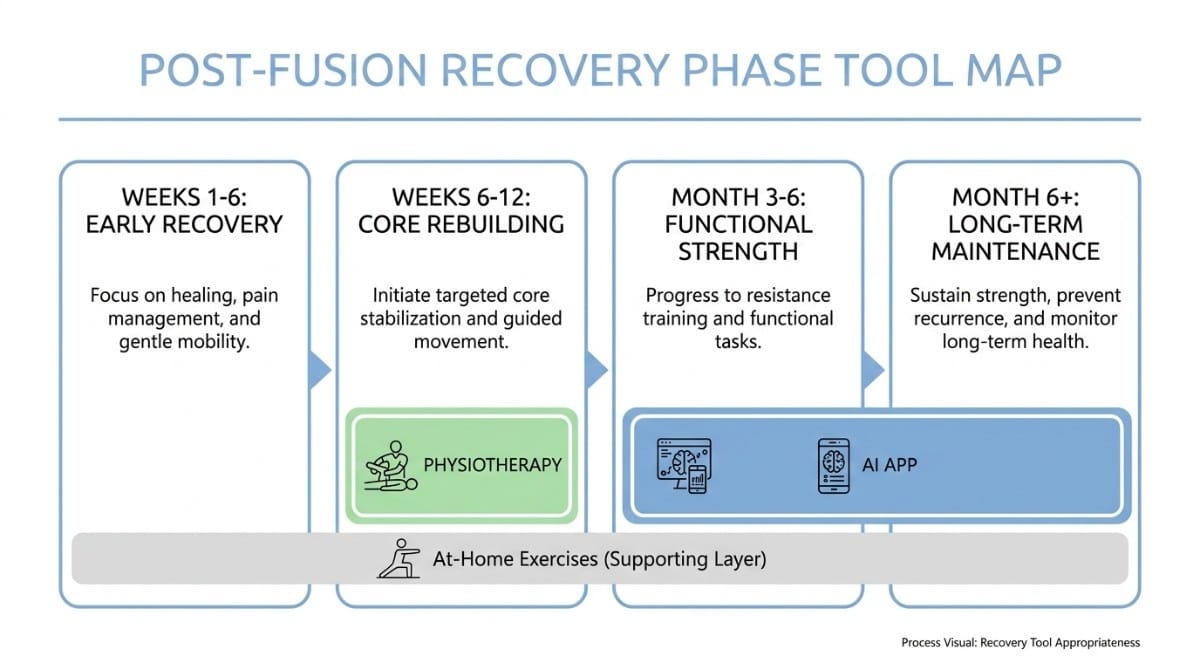
What the Research Says About Post-Fusion Rehabilitation
Physiotherapists often recommend a combination approach - formal supervision early in recovery, transitioning to self-managed exercise with accountability tools as independence increases.
Research in musculoskeletal rehabilitation consistently shows that:
- Supervised exercise programmes produce better short-term outcomes (weeks 6-16) than unsupervised exercise alone
- Long-term outcomes (12-24 months) are more strongly predicted by daily exercise consistency than by early clinical intensity
- Patients who use digital health tools to maintain exercise habits during the maintenance phase report better functional outcomes than those who stop formal rehabilitation without a replacement structure
Posture specialists suggest that the recovery gap - the period between completing formal physiotherapy and achieving full functional recovery - is where most patients lose ground. This is the phase AI-powered tools are specifically suited to fill.
If the pattern of pain returning during this gap is familiar, this breakdown of why back pain keeps coming back identifies the most common drivers and how to interrupt them.
The Combination Approach: What Best Practice Looks Like
No single method wins across the full recovery timeline. The most effective post-fusion rehabilitation programmes combine all three - sequenced appropriately.
Step-by-Step Recovery Framework:
Weeks 1-6 (Acute phase): Walking, breathing exercises, heel slides. No structured programme yet. Physiotherapy input is light and supervised.
Weeks 6-12 (Core rebuilding): Begin formal physiotherapy with a clinician who understands post-fusion protocols. Deep core activation, glute work, and neutral spine training. At-home exercises assigned and monitored by your physio.
Month 3-4 (Transition phase): Reduce physiotherapy frequency as independence increases. Begin using a structured AI recovery app (such as Backed AI) to maintain daily exercise habits, track posture, and progress the programme.
Month 4-6 (Functional strength): Continue AI-guided daily sessions. Introduce progressive resistance and functional movement. Return to physiotherapy for monthly check-ins if needed.
Month 6+ (Long-term maintenance): Daily posture and movement habits maintained through the app. Annual or bi-annual physiotherapy assessments as a quality check.
Tight hip flexors and glute weakness are among the most persistent issues during this maintenance phase - particularly for desk workers. This guide to hip flexor pain when sitting addresses exactly that pattern for people returning to desk-based work after fusion.
When This Approach Doesn't Work
The combination framework fails when:
- Physiotherapy is skipped entirely in the early phase and replaced too early with self-directed exercise
- At-home exercises are sourced from generic back pain content not designed for post-surgical spines
- AI app use begins before the patient can move independently and safely
- The patient alternates between intensive periods and complete rest - rather than consistent daily movement
- Underlying issues (poor sleep, ongoing smoking, nutritional deficiencies) are not addressed alongside physical rehabilitation
🚫 If pain at the fusion site increases during any exercise phase, stop immediately and contact your surgical team. Progressive neurological symptoms - numbness, tingling, weakness - always require urgent medical assessment.
Research & Expert Insight
Posture specialists and musculoskeletal rehab researchers increasingly agree that digital health tools are not a replacement for early clinical physiotherapy - but they are a highly effective bridge between the clinical phase and full independent recovery.
Final Takeaway
Spinal fusion recovery is a long game. The surgery takes hours. The rehabilitation takes months.
Physiotherapy is essential early - for safety, assessment, and structure. At-home exercises are necessary for daily frequency and long-term habit. AI posture tools fill the consistency gap that almost every post-fusion patient encounters during the middle and maintenance phases.
The patients who recover best are not the ones who work hardest in the first two weeks. They're the ones who show up consistently for six months.
Build a plan that supports that consistency - at every stage.
A Smarter Recovery Structure 📱
Backed AI is designed to fill exactly the gap that physiotherapy discharge creates.
Using your phone's camera, Backed AI analyses your posture, identifies compensatory patterns that develop during post-fusion recovery, and builds a personalised corrective exercise programme that adapts as you improve.
- 📊 AI posture scanning: Detects imbalances and compensation patterns specific to your recovery - not a generic population average
- 🎯 Adaptive programming: Your exercise programme evolves with your progress, maintaining the right challenge level throughout months 3-6 and beyond
- 🔄 Daily habit reminders: Short, focused sessions replace the willpower requirement of self-directed exercise - the single most common failure point in long-term recovery
Backed AI is not a replacement for your surgical team or your physiotherapist. It is the daily structure that keeps your recovery moving forward when clinical support steps back.
Download Backed AI and start correcting your posture today.
FAQ
Q1: Is physiotherapy necessary after spinal fusion surgery?
Physiotherapy is strongly recommended after spinal fusion, typically beginning at 6-12 weeks post-surgery with surgeon clearance. It provides clinical assessment, hands-on correction, and structured progression that cannot be safely replicated through self-directed exercise alone in the early recovery phase.
Q2: Can I do at-home exercises instead of physiotherapy after back fusion? At-home exercises are an important part of recovery but should not replace formal physiotherapy in the early phase (weeks 6-16). Generic home programmes carry a risk of incorrect form and inappropriate exercise selection for post-fusion patients. The safest approach combines physiotherapy for early structure with supervised at-home exercises for daily practice.
Q3: When can I start using an AI posture app after spinal fusion? Most post-fusion patients can begin using an AI posture and exercise app like Backed AI from approximately month 3 onwards - once the initial physiotherapy phase is complete and independent movement is safe. AI apps are most effective as a consistency and habit-building tool during the middle and maintenance phases of recovery.
Q4: What is the biggest risk of skipping rehabilitation after spinal fusion? The primary risk is adjacent segment disease - degeneration of the vertebrae above or below the fused segment due to incorrect load distribution. Without rehabilitation, the muscles that should support the fused segment remain weak, forcing adjacent vertebrae to absorb excess stress. This is one of the most common causes of ongoing pain after a structurally successful fusion.
Q5: Which recovery method produces the best outcomes after spinal fusion? Research consistently shows that a combination approach produces the best long-term outcomes: formal physiotherapy in the early structured phase, consistent at-home exercise throughout, and an AI-powered tool (such as Backed AI) to maintain daily habit and progression during months 3 onwards. The single strongest predictor of outcome is long-term consistency - not the intensity of any single phase.


