How to Stop Your Lower Back Pain Coming Back: The Long-Term Habits That Actually Stick

Getting out of lower back pain is one challenge. Staying out of it is another entirely. Most people manage the first - and then repeat the same patterns that caused the pain in the first place. This article is about building the habits that make relapse the exception, not the rule.
Preventing lower back pain from returning requires shifting from reactive treatment to proactive lifestyle habits - specifically, daily movement, postural awareness, sleep hygiene, and consistent strength maintenance that the body can sustain indefinitely.
TL;DR
- Most lower back pain returns because the root cause - posture, muscle imbalances, movement patterns - was never fully addressed
- Long-term prevention requires habit-level changes, not temporary fixes
- The five core habits are: daily movement, postural maintenance, sleep optimisation, load management, and consistency systems
- Lifestyle integration matters more than exercise intensity - 10 consistent minutes beats 60 occasional minutes every time
- Backed AI provides the ongoing structure and accountability that makes long-term consistency achievable
Why Lower Back Pain Keeps Coming Back
Understanding recurrence is the starting point for preventing it.
Lower back pain has one of the highest relapse rates of any musculoskeletal condition. Research consistently shows that 60-80% of people who experience a lower back pain episode will have at least one recurrence within a year - and many develop a chronic cycling pattern that persists for years or decades.
This is not bad luck. It is a predictable outcome of how most people approach recovery.
The typical pattern looks like this:
- Pain appears
- Person rests, takes pain relief, does some stretches
- Pain reduces
- Person returns to the same habits that caused the pain
- Pain returns - usually within weeks or months
The cycle breaks only when the underlying drivers are permanently addressed - not just managed during the painful phase.
As we explored in our guide to why your back pain keeps coming back, the physical cycle of pain, compensation, and recurrence is almost always rooted in unresolved muscle imbalances and postural patterns. Permanent prevention requires addressing these at the lifestyle level - not just during acute episodes.
💡 Key Insight: Most people treat lower back pain like a fire to put out. Long-term prevention requires treating it like a system to maintain - the way you maintain your car, your diet, or your sleep. The fire goes out. The system keeps running.
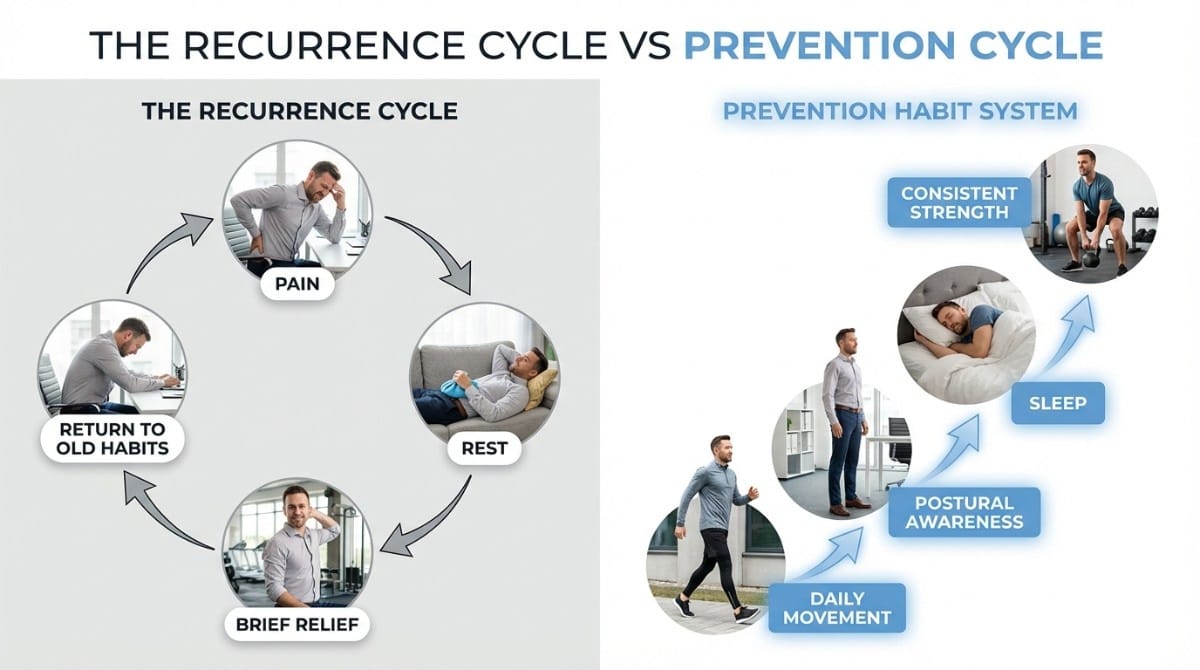
What Is Lower Back Pain Prevention?
Lower back pain prevention is not about avoiding all movement or treating your spine as fragile. It is the opposite.
Lower back pain prevention is the ongoing practice of maintaining lumbar spine health through daily movement habits, postural awareness, and lifestyle choices that keep the muscles, joints, and discs functioning optimally - reducing the probability of recurrence to near zero.
The spine is designed to move, load, and recover. Prevention is about giving it the conditions to do that reliably.
The 5 Core Habits That Stop Lower Back Pain Returning
These are not temporary interventions. They are permanent lifestyle integrations - small enough to sustain indefinitely, significant enough to change the long-term trajectory of your spinal health.
Habit 1: Daily Movement (Non-Negotiable)
The single most evidence-backed intervention for preventing lower back pain recurrence is consistent daily movement.
Not intense exercise. Not long sessions. Daily, consistent, targeted movement.
Physiotherapists often describe this as the difference between people who fix their back pain and those who don't. The fixers move every day. The relapsers exercise sporadically.
What this looks like in practice:
- 10-15 minutes of targeted lower back and hip mobility work each morning
- Movement breaks every 30-45 minutes during sedentary work
- At least one longer movement session (walk, swim, yoga, mobility class) 3-5 times per week
- No day of complete stillness - even on rest days, 10 minutes of gentle movement counts
The exercises themselves matter less than the consistency. A moderate routine done daily beats a perfect routine done twice a week.
For the specific exercise structure that works best for long-term lower back maintenance, our lower lumbar pain stretches guide provides a phased routine that adapts from acute relief to long-term maintenance.

Habit 2: Postural Maintenance
Fixing posture during a pain episode is reactive. Maintaining posture permanently is preventive.
The key distinction: posture maintenance is not about consciously holding yourself rigid all day. It is about training the muscles that make good posture the default - so it happens automatically, without effort.
The three postural habits with the highest prevention value:
Active sitting awareness The lower back should maintain a gentle inward curve when seated. This requires the lumbar support of a chair to be correctly positioned - and the hip flexors and glutes to be strong enough to support the pelvis in a neutral position. Check your seated posture three times per day. Not constantly - just three deliberate check-ins.
Ear-over-shoulder alignment when standing Forward head posture creates a compensatory chain that loads the thoracic and lumbar spine. When standing, the ear should be directly above the shoulder. This single check-in can reveal and correct chronic forward head loading before it cascades into lower back pain.
Anterior pelvic tilt correction The most common postural driver of lower lumbar pain. Stand sideways in front of a mirror. If your lower back is excessively curved and your stomach pushes forward, anterior pelvic tilt is present. The long-term correction requires consistent hip flexor stretching and glute strengthening - both of which belong in a daily routine. For a full breakdown of posture types and their lower back implications, see our guide to types of bad posture and what your body is telling you.
Habit 3: Sleep Optimisation for Spinal Recovery
The spine recovers during sleep. The discs rehydrate, the muscles repair, and the nervous system resets pain sensitivity. Poor sleep doesn't just feel bad - it actively compromises spinal recovery and lowers pain thresholds.
Sleep habits that protect the lower back:
Our detailed guide to best sleeping positions for lower back pain covers each of these factors in full, with specific position guidance for different pain patterns.
Habit 4: Load Management
Lower back pain prevention is not about avoiding load. The spine needs load to stay healthy - bone density, disc nutrition, and muscle strength all depend on appropriate mechanical stress.
The key word is appropriate.
Load management principles for long-term prevention:
Progressive loading Increase exercise intensity, weight, and duration gradually. The most common cause of exercise-related lower back pain recurrence is doing too much too soon after a pain-free period.
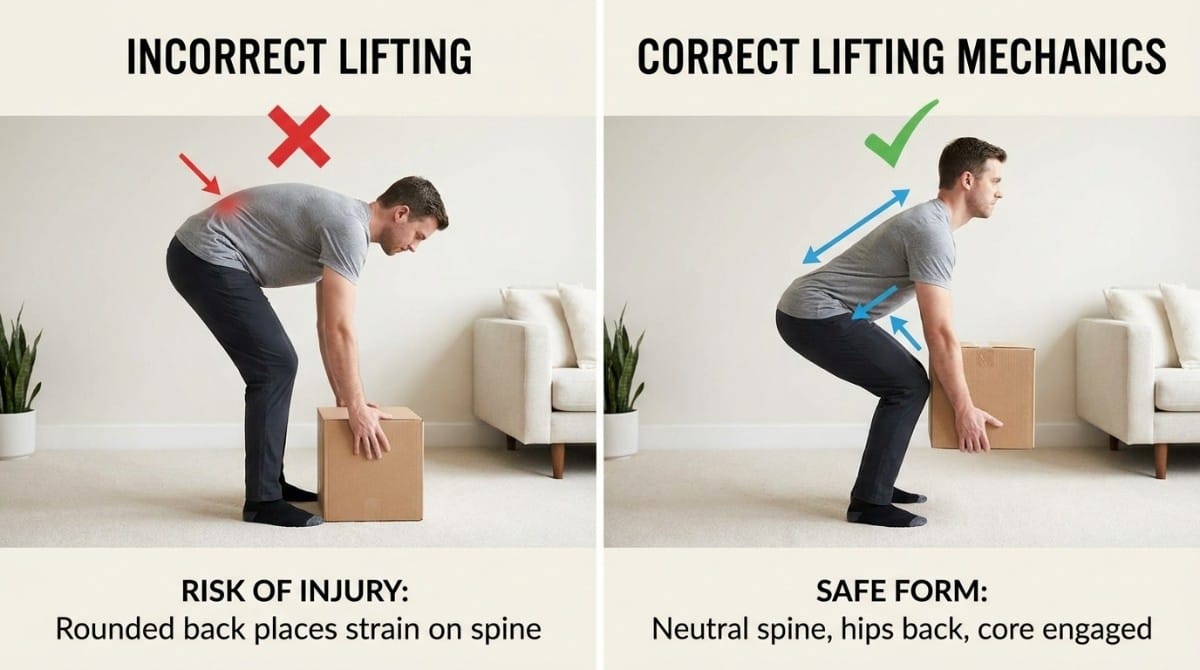
Lift mechanics The lower back is most vulnerable during forward bending under load with rotation - think picking up a heavy bag awkwardly. Establish correct lifting mechanics as a permanent habit: hinge at the hips, keep the spine neutral, engage the core before lifting.
Carry symmetry Asymmetric carrying - a heavy bag on one shoulder, a child always on one hip - creates uneven lumbar loading over time. Alternate sides, use backpacks for heavier loads, and be aware of habitual asymmetries.
Exercise variety Doing the same exercises indefinitely leads to adaptive shortening of some muscles and neglect of others. Rotate between mobility, strength, and endurance-focused movement across the week.
Habit 5: Build a Consistency System
The four habits above are straightforward. The challenge is not knowing them - it is doing them consistently when life is busy, when the pain has eased, and when motivation has faded.
Posture specialists suggest that the difference between people with chronic recurring back pain and those who have resolved it permanently is almost never knowledge. It is almost always system.
Building a consistency system:
Anchor habits to existing routines The morning mobility routine works best immediately after waking, before the busyness of the day creates friction. The evening stretching works best immediately before bed. Attaching new habits to existing anchors dramatically increases adherence.
Track progress visibly Seeing improvement - reduced pain scores, better range of motion, fewer bad days - is one of the most powerful motivators for continuing. Track weekly, not daily.
Use reminders during transition periods The highest-risk period for habit collapse is not during the painful phase - it is 4-6 weeks after recovery, when pain is low and the urgency of the habit feels reduced. Set calendar reminders or use an app with daily prompts specifically for this window.
Lower the activation energy A yoga mat left out in the living room is more likely to be used than one stored in a cupboard. Make the starting point of each habit as frictionless as possible.
Plan for disruption Travel, illness, busy work periods - these will disrupt your routine. The plan is not to be perfect. The plan is to have a minimum viable version of each habit ready for disrupted periods. Even five minutes of morning movement is better than zero.
How to Know If Your Prevention Habits Are Working
Prevention success is measured differently from pain treatment success. You are not chasing relief - you are chasing absence of recurrence and progressive improvement in baseline function.
Signs your prevention habits are working:
- Morning stiffness has reduced or disappeared
- You can sit for extended periods without significant aching building
- You move more freely - bending, reaching, and rotating without guarding
- Bad days are less frequent and less severe
- Recovery from a hard physical day is faster than it used to be
- You are not thinking about your back pain as a constant background concern
Signs a habit adjustment is needed:
- Pain is returning after previously improving
- You have stopped one or more of the five habits without replacing them
- Your movement routine has not progressed in 8+ weeks
- You are experiencing new pain patterns in adjacent areas (hips, knees, upper back) suggesting new compensation
When This Approach Doesn't Work
The lifestyle prevention framework above is designed for mechanical lower back pain - the vast majority of cases.
It is not sufficient as a standalone approach if:
- You have an inflammatory spinal condition (ankylosing spondylitis, rheumatoid arthritis affecting the spine)
- You have significant structural changes (severe disc degeneration, spinal stenosis, spondylolisthesis)
- Your pain has neurological features (consistent leg weakness, bladder or bowel changes)
- You are post-surgical and following a specific recovery protocol
In these cases, the habits above may still be appropriate - but should be implemented under the guidance of a physiotherapist or spinal specialist, not independently.
Step-by-Step: Building Your Long-Term Prevention Stack
Month 1: Foundation
- Establish the daily 10-15 minute morning mobility routine
- Implement movement breaks every 30-45 minutes during sedentary work
- Audit and correct your sleep position
Month 2: Strengthening
- Add progressive glute and core strengthening to your weekly routine
- Begin tracking pain scores and movement quality weekly
- Address any remaining postural issues identified in Month 1
Month 3: Integration
- Embed the five habits as non-negotiable daily anchors
- Introduce one additional weekly movement session (walk, swim, yoga)
- Assess progress: most people at this stage have significantly reduced or eliminated recurrence
Month 4 onward: Maintenance
- Continue the daily routine with progressive variation
- Review and upgrade exercises every 6-8 weeks to prevent adaptation
- Use the Backed AI programme to ensure the routine continues evolving with your body's changing needs

Research & Expert Insight
- Research in musculoskeletal rehabilitation shows that people who maintain a daily exercise routine after initial lower back pain recovery have a recurrence rate approximately 45% lower than those who return to a sedentary baseline
- Physiotherapists often recommend treating the post-recovery period as the highest-risk window for relapse - the 4-8 weeks after pain resolves when habits are most likely to be abandoned
- A 2022 systematic review in The Lancet identified physical activity, sleep quality, and psychological factors (stress, catastrophising) as the three strongest modifiable predictors of lower back pain recurrence
- Posture specialists suggest that anterior pelvic tilt correction and hip flexor maintenance are the two highest-value long-term interventions for preventing lumbar spine deterioration in desk-based adults
- Research consistently shows that self-management education combined with exercise produces better long-term outcomes than either intervention alone - the knowledge of why the habits matter increases adherence significantly
Final Takeaway
Lower back pain prevention is not a programme you complete. It is a system you maintain.
The five habits - daily movement, postural maintenance, sleep optimisation, load management, and a consistency system - are not complicated. They are small, sustainable, and cumulative. Done consistently over months, they transform the lower back from a recurring problem into a functioning, reliable part of your body.
The difference between people who fix their lower back pain permanently and those who remain in the recurrence cycle is not physiology. It is habit architecture.
Build the system. Trust the process. The results accumulate.
For desk workers specifically, our guide to lower back pain for desk workers provides the specific daily routine most relevant to sedentary work environments.
Why Most Prevention Attempts Fail
Most people who successfully recover from lower back pain do not maintain the habits that got them there.
The pain fades. The urgency fades with it. The routine quietly disappears over 4-6 weeks. Then the pain returns - and the cycle begins again.
This is not a willpower failure. It is a system failure.
Without ongoing structure, reminders, and progression, long-term prevention habits collapse under the weight of ordinary life. The solution is not more motivation. It is a better system.
Why Most Exercise Plans Fail
- No adaptation - the same routine at month six as month one means the body has adapted and stopped responding
- No accountability - nothing prompts you when life gets busy and the habit starts slipping
- No progress visibility - without tracking, improvement becomes invisible and motivation fades
- No personalisation - a generic prevention plan doesn't know your specific postural pattern or which habits matter most for your body
The Prevention System That Keeps Working
Backed AI is not just a recovery tool. It is a long-term posture and movement maintenance system.
- 📱 AI posture scan - identifies your specific lumbar pattern and updates your programme as your posture improves over time
- 🎯 Adaptive personalised programme - exercises evolve with your body. What you need in month one is different from what you need in month six. Backed AI adjusts automatically
- ⏰ Daily habit reminders - the consistent prompt that keeps the routine alive during busy periods and after the urgency of pain has faded
- 📈 Long-term progress tracking - see measurable improvement week by week, month by month. Progress visibility is one of the strongest habit reinforcers known to behavioural science
Whether you are three weeks out of an acute episode or six months into a maintenance routine, Backed AI gives you the structure that makes consistency the default - not the exception.
Download Backed AI and start correcting your posture today.
FAQ
Q1: How do I stop my lower back pain from coming back permanently?
Permanent prevention requires addressing the root causes - not just managing symptoms. The five core habits are: daily targeted movement, postural maintenance, sleep optimisation, appropriate load management, and a consistency system with reminders and tracking. All five together, sustained over months, dramatically reduce recurrence risk.
Q2: How long does it take to prevent lower back pain from returning?
Most people who establish consistent daily movement and postural habits see a significant reduction in recurrence frequency within 6-8 weeks. Full stabilisation - where the lower back is functionally reliable and pain-free as a baseline - typically takes 3-6 months of consistent practice.
Q3: Is daily exercise necessary to prevent lower back pain?
Yes - daily movement is the single most evidence-backed intervention for lower back pain prevention. It does not need to be intense or long. Ten to fifteen minutes of targeted mobility and strengthening work, done consistently every day, outperforms longer sessions done sporadically.
Q4: What is the biggest mistake people make after recovering from lower back pain?
Returning immediately to the same habits that caused the pain in the first place. The 4-6 weeks immediately after recovery - when pain has resolved and urgency is low - is the highest-risk period for habit collapse and relapse. This is the period where a consistency system matters most.
Q5: Can lower back pain be prevented long-term without seeing a physiotherapist?
For mechanical lower back pain - the most common type - yes. A structured daily routine addressing hip flexor flexibility, glute strength, lumbar mobility, and core stability, combined with postural awareness and sleep habits, can prevent recurrence without ongoing clinical visits. Apps like Backed AI provide the personalisation and structure that make self-managed prevention effective.


