Why Does My Lower Lumbar Hurt? Causes, Triggers, and What Your Body Is Telling You

Lower lumbar pain is one of the most common physical complaints adults experience - but most people don't know why it's happening to them specifically. Understanding the cause of your pain is the first and most important step toward fixing it for good.
Lower lumbar pain is discomfort, aching, or stiffness in the lowest section of the spine (vertebrae L1-L5), typically caused by muscle imbalances, postural dysfunction, or repetitive mechanical stress rather than structural damage.
TL;DR
- The lower lumbar spine (L1-L5) carries more load than any other spinal region
- Most lower lumbar pain is mechanical - caused by muscles, posture, and movement patterns
- The most common causes are prolonged sitting, weak core, tight hip flexors, and poor spinal alignment
- Pain patterns (morning vs evening, sitting vs standing) reveal a lot about the root cause
- Ignoring it leads to compensation injuries and chronic pain cycles
- Backed AI can identify your specific posture pattern and build a targeted recovery plan
What Is the Lower Lumbar Region?
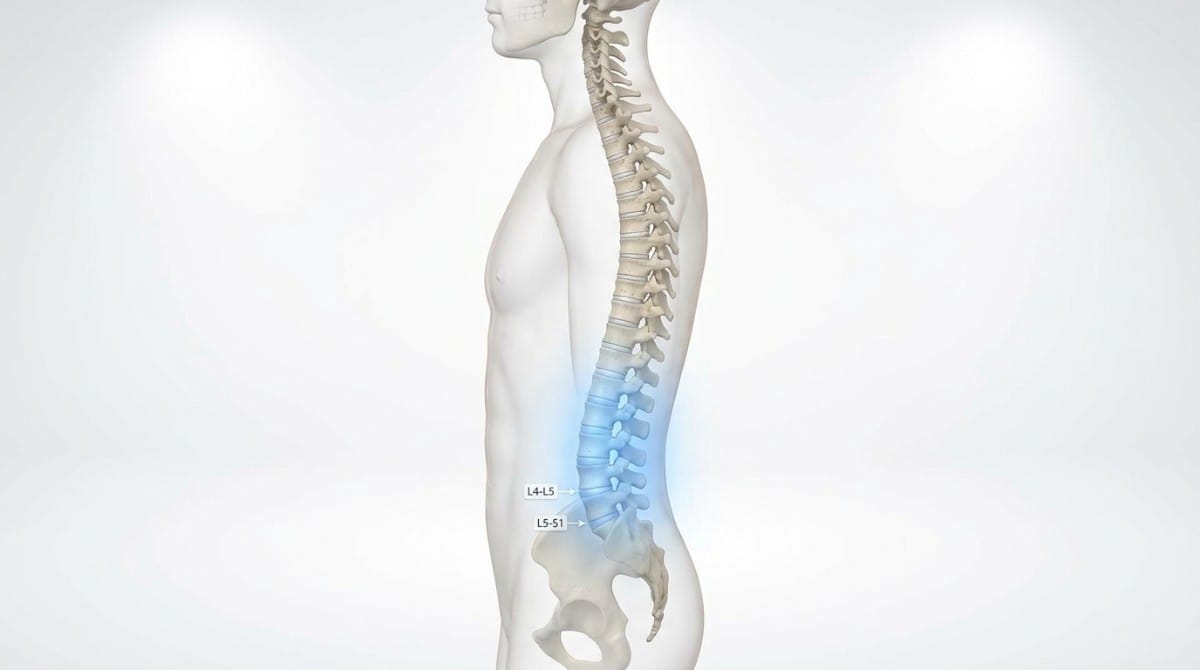
The lumbar spine sits between the ribcage and the pelvis. It has five vertebrae - L1 through L5 - and is responsible for supporting most of your body's weight while allowing you to bend, twist, and move.
The lowest two segments - L4-L5 and L5-S1 - are the most commonly affected in people with lower back pain. These joints absorb enormous force during daily activities, from sitting at a desk to picking something off the floor.
The lumbar region is supported by layers of muscle, fascia, and connective tissue. When any part of that support system weakens or tightens unevenly, the spine compensates - and that's when pain begins.
What Causes Lower Lumbar Pain?
Lower lumbar pain has many possible causes. Most fall into two categories: mechanical (how you move and hold your body) and structural (physical changes to the spine itself).
The vast majority of cases - estimated at over 85% by musculoskeletal researchers - are mechanical. That means they are fixable with the right approach.
The Most Common Causes
1. Prolonged Sitting Sitting compresses the lumbar discs and shuts off the glutes and core muscles that protect the spine. Over time, this creates a pattern where the lower back muscles overwork to compensate - leading to chronic tension and pain.
2. Weak Core and Glutes The lumbar spine relies on surrounding muscles to stay stable. When the core and glutes are weak or inactive, the lower back absorbs excess load. This is one of the most common and overlooked drivers of lower lumbar pain.
3. Tight Hip Flexors Tight hip flexors pull the pelvis forward into anterior pelvic tilt - which increases the curve of the lower lumbar spine and compresses the lumbar joints. This is extremely common in people who sit for long hours. Our detailed guide on tight hip flexors and lower back pain explains this mechanism in full.
4. Poor Posture Patterns Habitual postural deviations - such as flat back posture, anterior pelvic tilt, or forward head posture - alter the distribution of load across the lumbar spine. None of these are comfortable long-term. For a full breakdown of how different posture types affect the spine, see our guide to types of bad posture and what your body is telling you.
5. Muscle Imbalances When some muscles are overactive and tight while others are weak and underused, the lumbar spine is pulled out of alignment. The most common imbalance pattern: tight hip flexors and erector spinae paired with weak glutes and deep core.
6. Repetitive Movement Patterns Repetitive bending, lifting with poor form, or even walking with an uneven gait can stress the lumbar joints over time. This is common in manual workers and athletes alike.
7. Disc-Related Issues A bulging or herniated disc at L4-L5 or L5-S1 can cause localised lumbar pain as well as radiating pain down the leg (sciatica). This is a structural cause and typically requires professional assessment.
What Your Pain Pattern Is Telling You
Not all lower lumbar pain is the same. When and how your pain presents gives important clues about the root cause.
| Pain Pattern | Most Likely Cause |
|---|---|
| Worst in the morning, eases with movement | Muscle stiffness, disc pressure from sleep position |
| Worse after sitting for long periods | Hip flexor tightness, lumbar disc compression |
| Worse when standing for a long time | Anterior pelvic tilt, weak glutes, lumbar hyperextension |
| Aching during or after exercise | Muscle overload, poor form, weak core support |
| Sharp pain with bending or twisting | Possible disc involvement or facet joint irritation |
| Pain that radiates down one leg | Nerve involvement - seek professional assessment |
| Pain that improves with movement | Mechanical origin - stretching and exercise will likely help |
💡 Key Insight: If your lower lumbar pain improves when you walk around and worsens after stillness, that's a strong signal the cause is mechanical - and that movement-based recovery will work well for you.

Why Does Lower Lumbar Pain Come Back?
Many people experience lower lumbar pain, feel better after a few days of rest, and assume the problem is solved. Then it returns - often worse.
This cycle happens because:
- Rest treats the symptom, not the cause. The muscle imbalance, posture pattern, or movement habit that created the pain is still there.
- Compensation patterns develop. When the lower back hurts, surrounding muscles adapt to protect the area. These compensations create new tension points that perpetuate the cycle.
- The core and glutes never get properly reactivated. Resting switches these muscles off further. Without targeted rehab, they stay weak.
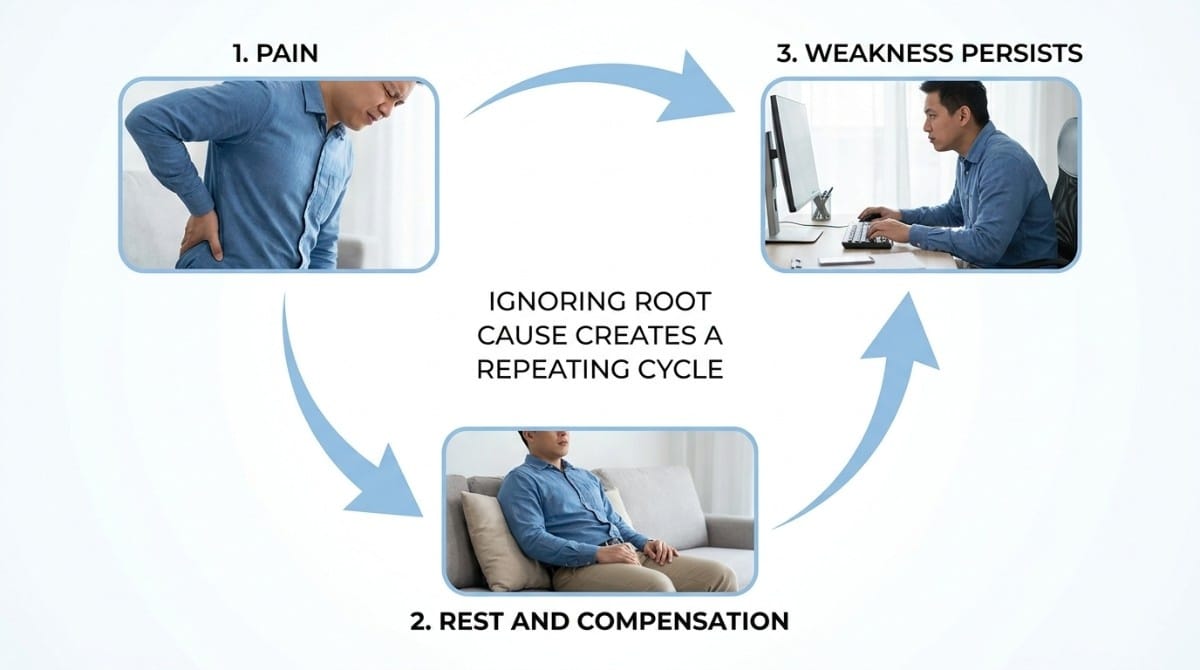
Physiotherapists often describe this as the pain-weakness-compensation cycle - and breaking it requires addressing the root cause, not just the pain signal.
For a full breakdown of this cycle and how to escape it, see our article on why your back pain keeps coming back.
How Posture Directly Affects the Lower Lumbar Spine
Your resting posture determines how much load your lower lumbar spine carries all day - before you've even moved.
Anterior pelvic tilt increases the lumbar curve (lordosis), compressing the facet joints at L4-L5 and L5-S1. This is the most common postural driver of lower lumbar pain.
Flat back posture reduces the natural lumbar curve, placing excessive stress on the lumbar discs rather than distributing load across the joints.
Forward head posture - while primarily a neck issue - creates a compensatory chain that increases tension across the thoracic and lumbar spine.
In all three cases, the lower lumbar region ends up absorbing stress it was never designed to carry continuously.
Understanding your specific posture pattern is essential. A generic approach to lower back pain won't work if your specific posture type is contributing to the problem in a unique way.
Research & Expert Insight
- Research in musculoskeletal rehab shows that 80-90% of lower lumbar pain cases are non-specific mechanical in origin - meaning no identifiable structural damage, and directly linked to posture and movement habits
- Physiotherapists often recommend addressing hip flexor tightness and glute weakness as primary targets in lumbar pain recovery - not just the lumbar muscles themselves
- Posture specialists suggest that anterior pelvic tilt is present in the majority of desk-worker lower back pain cases, and correcting it is key to lasting relief
- A 2022 study published in the Journal of Orthopaedic & Sports Physical Therapy found that adults who corrected lumbar alignment through targeted exercise programmes reported a 52% reduction in pain recurrence over 12 months
What Happens If Lower Lumbar Pain Goes Untreated?
Short-term neglect is common. Long-term neglect is costly.
Within weeks:
- Muscle compensation patterns become habitual
- Range of motion decreases
- Simple movements (bending, lifting) become risk events
Within months:
- Pain transitions from acute to chronic (lasting more than 3 months)
- Sleep is disrupted by discomfort
- Mood and energy are affected - chronic pain has well-documented psychological impact
Over years:
- Disc degeneration can accelerate at L4-L5 and L5-S1
- Adjacent joints compensate, creating secondary pain sites
- Recovery becomes more complex and time-consuming
The earlier you understand the cause and address it, the faster and more complete your recovery will be.
When This Approach Doesn't Work
The educational framework above applies to mechanical lower lumbar pain - the most common type.
Seek professional medical assessment if:
- Pain is severe (7/10 or above) and not improving after 2 weeks of gentle movement
- You experience pain radiating down one or both legs
- You notice numbness, tingling, or weakness in the legs or feet
- Pain began after a fall, accident, or significant physical trauma
- You have unexplained weight loss alongside back pain
- Pain is worse at night and unrelated to movement
These signs may indicate a structural or systemic cause that requires clinical investigation.
Step-by-Step: How to Identify Your Lower Lumbar Pain Cause
Step 1 - Map your pain pattern Use the table above to identify when your pain is worst and what activities trigger or relieve it.
Step 2 - Assess your posture Stand sideways in front of a mirror. Is your lower back excessively curved? Does your stomach push forward? This suggests anterior pelvic tilt.
Step 3 - Test your hip flexors Lie flat on your back. Can you press your lower back fully into the floor without arching? If not, your hip flexors are likely tight.
Step 4 - Test your glute activation Lie on your back, feet flat. Perform a glute bridge. Do your hamstrings cramp instead of your glutes activating? This indicates glute inhibition - a key lower back pain driver. Our guide to glute activation exercises walks you through how to fix this.
Step 5 - Begin targeted recovery Once you've identified your pattern, begin a routine that addresses the specific cause - not a generic lower back protocol.

Final Takeaway
Most lower lumbar pain has a mechanical cause - and mechanical causes respond well to targeted movement, posture correction, and consistent rehab.
The key is identifying your specific pattern rather than applying a generic solution. Pain that's worst in the morning points to a different cause than pain that builds through a long day of sitting. Treatment should match the trigger.
Once you understand your cause, the path forward becomes much clearer. If you're ready to start with stretches and relief exercises, our lower lumbar pain stretches guide covers 10 safe moves structured around a phased recovery plan.
Why Most People Never Fix Their Lower Back Pain
Most people know their lower back hurts. Very few know exactly why.
Without knowing the cause - whether it's anterior pelvic tilt, weak glutes, tight hip flexors, or a postural pattern that's been building for years - any exercise routine becomes a guess. Some guesses help. Many don't. And the cycle continues.
Why Most Exercise Plans Fail
Generic lower back routines fail for predictable reasons:
- No diagnosis - they treat the pain location, not the cause
- Wrong exercise selection - stretching a muscle that needs strengthening, or vice versa
- No progression - the body adapts and the routine stops working
- No consistency - without structure and reminders, most people quit within 10 days
Get a Plan Built Around Your Posture Pattern
Backed AI starts where most programmes don't - with an understanding of your specific posture.
- 📱 AI posture scan identifies your lumbar alignment, pelvic position, and postural type in minutes
- 🎯 Personalised programme targeting the exact muscles contributing to your lower lumbar pain
- 📈 Progress tracking so you can see measurable improvement - not just hope for it
Rather than guessing which stretch might help, Backed AI shows you exactly what your body needs - and builds the daily habit that makes recovery stick.
Download Backed AI and start correcting your posture today.
FAQ
Q1: What is the most common cause of lower lumbar pain?
The most common cause is mechanical dysfunction - including muscle imbalances, tight hip flexors, weak glutes and core, and postural deviations like anterior pelvic tilt. Structural causes like disc herniation account for a smaller proportion of cases.
Q2: How do I know if my lower lumbar pain is serious?
Seek professional assessment if pain is severe (7/10 or above), radiates down your leg, causes numbness or tingling, or doesn't improve after two weeks of gentle movement. These signs may indicate nerve involvement or a structural issue.
Q3: Why is my lower lumbar pain worse in the morning?
Morning lower lumbar stiffness is typically caused by reduced circulation and fluid redistribution in the spinal discs during sleep. It often eases within 20-30 minutes of gentle movement and is usually a sign of mechanical rather than structural pain.
Q4: Can poor posture cause lower lumbar pain?
Yes. Anterior pelvic tilt, flat back posture, and prolonged sitting all alter how load is distributed across the lumbar spine. Over time, these patterns create muscle imbalances that lead to chronic lower lumbar discomfort.
Q5: Is lower lumbar pain the same as sciatica?
No, but they can overlap. Lower lumbar pain refers to localised discomfort in the lumbar region. Sciatica involves the sciatic nerve and typically causes pain, tingling, or numbness radiating from the lower back down one leg. Sciatica is often caused by a disc issue at L4-L5 or L5-S1.


